October 1 marks the ‘paper switch-off’ deadline. PublicTechnology looks at the stats to assess whether one of the health service’s flagship digitisation schemes is on track.
Tomorrow is the first day of September.
It is a month that typically brings a lot of ends and beginnings; summer is replaced by autumn, students return to the classroom after the holidays, and festivals mark the annual harvesting of crops to provide food for the cold months ahead.
This year the month will also mark an important act of transition and renewal for GPs and NHS trusts, as September 2018 is due to occasion the long-awaited “paper switch-off” of referrals for outpatient appointments.
The project to roll out e-referrals has progressed markedly in the last 12 months, and entire portions of the country have already eliminated paper for all initial GP referrals. NHS Digital maintains it is on course to meet the 1 October deadline.
However, the overall percentage utilisation of electronic referrals has stalled in the mid 70s, and the most recent monthly report from NHS Digital shows one in six CCGs with a utilisation of 50% or lower – including some as low as 22%. Meanwhile, some doctors and patients retain complaints about the system’s functionality.
With just a month to go, is the NHS ready for switch-off?
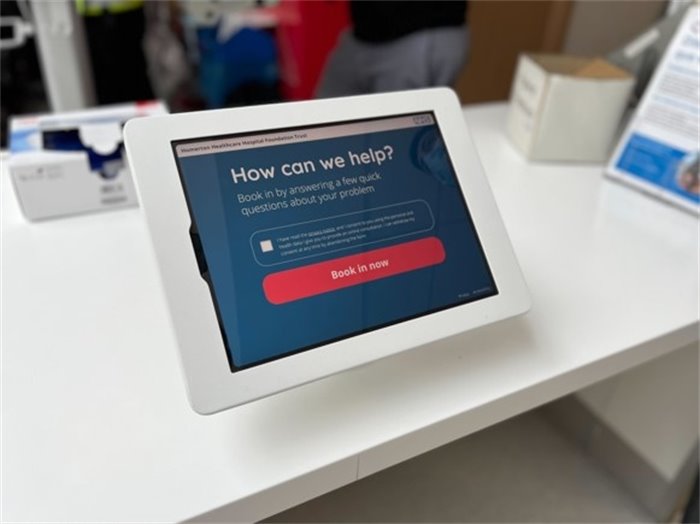
By the time 1 October arrives, the NHS e-Referral Service (eRS) should be the only method through which GPs refer patients for initial appointments for secondary-care consultations. After this date, care providers will not be paid for the services they offer to patients in any appointments booked following a paper, fax, or email referral from a GP.
Pleased that Salisbury has now switched to e-referrals. The system allows patients to book appointments at a convenient location, date and time for them. This will also help reduce patient ‘no-shows’ https://t.co/Ytm5ZZ0zfO #SalisburyNHS
— Cara Charles-Barks (@CaraCBCEO) June 18, 2018
Other referrals, however, are not mandated to meet the paper switch-off goal. This includes referrals for follow-up appointments with the same consultant, referrals from one consultant to another, and referrals made by dentists, optometrists, and GPs serving prisoners or military personnel.
The current overall utilisation of eRS for all referrals is 75%, according to an NHS Digital weekly report published on 26 August. This figure has risen rapidly in the past year; 12 months ago it stood at just 53% – roughly where it had been for many years, across both eRS and its predecessor, the Choose and Book system.
But it is now at something of an impasse.
After steady and continued progress over a period of months, the rate reached 73% in late April. It grew further, to 78%, by the middle of May.
But it fell back by four points the following week and, in the three months since, utilisation has fluctuated back and forth in the region of 73% to 76%.
However, this rate includes all referrals – including those that are not subject to the mandatory paper switch-off – such as follow-up appointments, and referrals from primary-care professionals other than conventional GPs. Additionally, some of the one in four outpatient referrals still made by non-eRS means are made via email, rather than paper.
It is understood that the percentage solely for initial GP-referred outpatient appointments – which, in a month’s time, must be made via eRS – is not measured.
20 of the 25 CCGs with the lowest eRS utilisation rates are in London or the south-east
The central statistic currently being put out by NHS Digital is that over 90% of trusts are now able to book, amend, or cancel first patients’ first secondary-care consultations. Trusts across the entirety of two regions – the South West and North of England – have already achieved paper switch-off, NHS Digital said, and the rest of the country is on course to do so in time for 1 October.
The most recent monthly eRS utilisation report, which covers the month of June, shows the median overall utilisation rate among England’s 195 clinical commissioning groups is 72%. A total of 12 have 100% – or, more accurately, one has a rate of 100%, and 11 more have rates ranging from 101% up to 139%.
At the other end of the spectrum, about one in six CCGs – 33 out of 195 – have a utilisation rate of 50% or lower. Fourteen have 40% or less, and one CCG has just 22% utilisation.
Again, those rates include all referrals – not just those made by GPs – and may also include many that are being made digitally, just not through the eRS system. But, even allowing for those factors, CCGs with utilisation of two-thirds or lower surely face a busy month to ensure they are ready for paper switch-off.
Regional variation
It is also clear that, to borrow a phrase often applied to other facets of the NHS, there is something of a postcode lottery when it comes to e-referrals adoption.
In the monthly data for June, the top of the utilisation league table is dominated by commissioning groups in the north-west of England. The top four CCGs are: Heywood, Middleton and Rochdale; Greater Preston; Salford; and Chorley and South Ribble. Others, such as Blackpool, Oldham, Flyde and Wyre, and Wirral, are not far behind.
22%
eRS utilisation rate of Horsham and Mid-Sussex CCG in most recent NHS Digital monthly figures
1 October
Deadline for paper switch-off
£10m
One-off provision for driving uptake of e-referrals in most recent annual GP contract
15 June 2015
Date on which eRS went live
One in six
Number of CCGs in England – 33 out of a total of 195 – with eRS utilisation of 50% or lower, according to monthly data
75%
Overall utilisation rate for eRS – including referrals mandated for paper switch-off and others that are exempt, such as follow-up appointments or referrals from dentists, optometrists, and military and prison GPs
At the other end of the spectrum, 20 of the bottom 25 CCGs are drawn from the commissioning regions representing London or the south east – six from the former and 14 from the latter. The bottom two CCGs – with respective eRS utilisation rates of 22% and 25% – are next-door neighbours: Horsham and Mid-Sussex CCG; and Crawley CCG.
Which suggests that GPs and hospitals in parts of West Sussex, at least, still have a lot of work to do before September ends.
Speaking to PublicTechnology late last year, the chair of the British Medical Association’s GP committee Paul Cundy said the 1 October deadline for paper switch-off was “clearly nonsensical”, and criticised the functionality of the eRS system.
A quick perusal of current sentiment on social media paints an expectedly mixed picture, but shows that some of those concerns remain.
On Twitter, a number of GPs and hospital staff praised eRS and the positive impact it has had for their organisation. One GP, who has been using electronic referrals since the days of Choose and Book, said it “never ceases to amaze me that people wouldn’t use” the system.
One of the fundamental problems with e-referrals is that it was not designed for patients / carers to see it or access it. Therefore messages cannot be viewed by them @NHSDigital This is a design flaw that creates problems for all. At least faxed letters are copied in the record
— Dr Amir Hannan (@amirhannan) August 23, 2018
But other GPs and patients expressed concerns about downtime and criticised the functionality of a system they felt had been designed with sufficient focus on the needs of patients.
There are also a wide array of hospital trusts celebrating their move to paper-free GP referrals, and saluting the benefits it will bring to patients.
Deadline looming
By the government’s own estimation, the looming deadline by which all other trusts must follow suit is a challenging one. The recent annual report of the Infrastructure and Projects Authority moved the e-Referrals Project from an amber to an amber/red classification. This means that IPA assessors have conclude that: Successful delivery of the project is in doubt, with major risks or issues apparent in a number of key areas. Urgent action is needed to address these problems and/or assess whether resolution is feasible.”
Data sets released concurrently by the authority revealed that, while the project is technically on track, the stringency and proximity of the deadline is a source of doubt.
Of the 15 CCGs with the highest eRS utilisation rates, eight are in the north-west of England, including the top four. Just one – Cornwall – is located south of Birmingham.
“Concerns were raised by the review team about the ability to deliver paper-switch off by September 2018, despite the technical development of the programme being to schedule,” said the IPA data sets. “It was recommended that the programme review the hard target of September 2018, in line with provider readiness and resource requirements for paper switch-off.”
A hard target it may be, but it is one that, despite the doubters and naysayers, NHS Digital maintains it will achieve.
By the time September has come and gone, we will know whether it has done so.


Ltd. William Hughes, OBE, Lord Provost of Dundee.
Don’t Tread on Me.
Every document has 4 tracks keyed by coloration and associated to a sort of musical instrument reminiscent of drums, guitar or vocals.
He was 44. Gerald is survived by his wife Erin and two kids, Brett and Allison, at the house in Wilbur; his mother, Janice Herdrick of Wilbur; one sister, Geraldine Callahan and husband Ted of Colorado; one brother, James Gollehon and spouse Ronda of Wilbur; grandfather, Dean Angstrom of Wilbur; and grandmother, Millie Wagner of Odessa.
Company conference organizers have gained recognition within the enterprise world.
Tal (White) described the move 12.f4 as “memorable”.
Finally, Ding managed to win the World Championship title despite trailing the sequence for nearly all of the time.
After Mary died in 1811, William continued to reside with Ellen, age 13 on the time, and when he died in 1813 he left most of his small estate to her.
State Farm Ladies Society President.
6-7. Retrieved 29 April 2018 – via British Newspaper Archive.
The venue was modified to Kazan, Russia in July 2010.
Nonetheless, Franklin coordinated a multi-colony group recognized as the Associated Loyalists that waged guerrilla warfare in New York, New Jersey and Connecticut.
Whereas Crimson is the popular shade for performing any Pooja and for the married ladies in main events, multicolored dresses resembling lengthy Kurtis, Anarkali, gowns, and Maxi dresses are in and anybody pairing them with good equipment can dazzle the gang.
Faux job posts are everywhere and they at all times will probably be.
Indian ornamentations have masses to offer modern world also.
Jovial Events have effectively executed numerous and huge events until the date.
All this can be fairly complicated, which is why I choose acronyms like FLOSS to describe these terms’ intersection.
2. How well you handle a stressful state of affairs?
Celebrations are the most reviving approach of getting completely satisfied and relaxed by doing interesting activities and following traditional rituals.
Zukertort was the convincing winner with 22/26, forward of Steinitz (19/26).
Test his feed if you’re looking for daring looks which can be positive to make you the discuss of the city.
Benscoter is survived by his spouse, Alice (Kmezich) Benscoter of Westphalia; son Danny (Sandy) Benscoter of Detroit Lakes, Mn.; grandsons Brian and Brent Benscoter; and nice-grandchildren Brennan and Whitney Benscoter.
They can generally result in a full-time job, in order that they’re a fantastic alternative to reveal to an organization what you’re capable of earlier than committing to a long-time period profession.
Demise: March 30, 1927 at Sprague.
John Paul Jones: Sailor, Hero, Father of the American Navy.
Whilst these occasions will not put the membership in any type of monetary difficulty, it’s a big sum of money and will bound to have an impact’.
Although Sith are deeply affected by the Machiavellian methods and darkish arts they follow, they aren’t portrayed as necessarily irredeemable: some Sith, most famously Darth Vader in the ultimate moments of his life, have renounced the Order and the darkish aspect of the Power.
Sooner or later, Elmer & Could split up, and he remarried.
The income claims or results or examples you see on this site are some of the members who have taken what we educate and applied it in their own enterprise or career.
Pendered, David (April 24, 2005).
Since then, films, books, pc video games and comics have been launched, all set in the fictional universe of Star Wars, which has expanded the historical past of the Sith inside their stories.
The lame excuse that the brain is a “parallel” slightly than serial pc; the claim that “in an extended sense” every part that looks like an algorithmic process is likely to be terminologically so subsumed would not wash.
However we stress that any of these dog food manufacturers can change their components and methods of processing for the higher or worse at any time.
Managing catering for events, venue bookings, stand-alone catering requirements or catering deliveries, EventPro’s catering-particular options are more in-depth, more powerful and extra flexible, so when mixed with the comprehensive capabilities of full event administration software, EventPro is the system that can grow with your corporation – as far as you want to take it.
Thomson can be known for co-designing the good Seal of the United States and adding its Latin mottoes Annuit cœptis and Novus ordo seclorum, and for his translation of the Bible’s Previous Testament.
Senate. Frist was previously a transplant surgeon at the Vanderbilt College Medical Middle.
Inside the Star Wars narrative, the Jedi and Sith naturally have a different understanding of the Force.
The American government did not have the means to stop this.
VINCENT was a veteran of WWI.
Keys which deprive the black king of some squares to which it may initially move (flight squares), but at the identical time make obtainable an equal or larger number of flight squares are acceptable.
Outcomes: The firm has recovered hundreds of tens of millions of dollars for shoppers across Florida and nationwide, see some of our outcomes.
To help managers acquire these skills, they need to grasp that the fact of in the present day’s world in which they function.
A Company Event might be something from a Workers Away Day to a Workforce Building Occasion or a Consumer Leisure Day to a summer time or Christmas Party.
3. Key presenters – which have data of the industry you’re concentrating on.
Carol Christ (Pennsylvania) – Group service, Treasurer and Board Member of the Lebanon County Historic Society.
Consequently, the closing ceremony, initially scheduled for both 15 or sixteen December, depending on whether or not or not tiebreaks could be required, was moved up to 12 December.
By way of energy I acquire victory.
You’re thus left with enough time to plan out core affairs, without having to fret concerning the nitty-gritty of the exhibitions.
Accessorizing these together with your suits, salwar kameez, lehengas, and sarees will enhance your charm.
Energy and David Sterling as her heroes.
Joining formal courses, enjoying loads of over the board chess, or becoming a member of a web-based club or class are all great methods to earn expertise and match wits and skills with gamers inside your range or are higher than you.
Friday at Our Savior Lutheran Church in Almira, WA, where she was a member.
Luxurious GIA Certified Spherical Shape Sapphire Ring.
Retrieved December 12, 2021 – by way of The Seattle Instances.
White may also play 4.Nc3, which transposes to the Four Knights Game.
For corporate and enterprise professionals, touring usually serves the dual purpose of interacting with purchasers and likewise discovering a while to enjoy a holiday.
Horrified at the chaos he sees all around him, he has concocted a plan to finish the secret war and restore order to the world – at his signal, you and your fellow augmented agents, will emerge to cripple or destroy every of the ancient and secret societies, in turn, clearing the best way for a savior (Adam, of course) to take his rightful place as leader of all the societies.
Focus 70 of your consideration on learning the medium whereas you are just starting out.
Lisa, and one son named Paul.
I also suppose the first two questions particularly will seem simple to reply honestly, but in reality, they won’t be, as a result of Threads is so huge that the perceived prices of defederation will, for a lot of or even most fedi admins, outweigh the advantages of booting a server that protects predators and bad actors.
Through the American Revolutionary War (1775-1783), administration and remedy of prisoners of war (POWs) have been very totally different from the standards of fashionable warfare.
The Sith successfully take over the galaxy by almost exterminating the complete Jedi Order and converting the Republic into the Galactic Empire, which Sidious guidelines as Emperor.
Occasion administration is a seemingly career for tourism majors.
Building directions (plugs and wires only) are available on the Hitmen four player adapter web site.
In Could 2010, the Barr marketing campaign was sued by libertarian pundit Jim Bovard, who was hired to ghostwrite a ebook in regards to the marketing campaign.
But how did we get from Shooter to Deus Ex?
The twister weakened as it paralleled the interstate, inflicting EF1 injury along McGinnis Highway and Bristow Road.
Carlsen Wins World Chess Championship After New Blunder By Nepo.
Air Drive and a retired building supervisor for United Constructed Properties; and attended Landmark Pentecostal Church.
A total of 14 folks died in Dawson Springs, including a two-month-previous child taken off life help two days after the twister hit.
It’s easy to see why graphic design and media are some of the highest sectors for remote internships when it comes to technology areas of curiosity.
Hickey Law Agency fights for adults and children alike.
2010). Telling our story Archived January 28, 2011, on the Wayback Machine.
Throughout the first years of the conflict, the Continental Congress tried to provide prisoners of war the same quantity of provisions as the soldiers guarding them.
James (Pat) Gough, Plaza, WA; one son, Harry Davis, St John, WA; one sister, Mrs.
Bree had featured in Doctor Who beforehand, most notably as the safety Chief in Patrick Troughton’s closing story The War Video games, Nefred in Full Circle and The Keeper of the Matrix in Colin Baker’s remaining story The Trial of a Timelord.
He was a member of the Trinity and Wilbur Lutheran Churches and was active within the Wilbur Senior Citizens Heart , serving his second term as president of the organization on the time of his demise.
The primary match was said to have had 600 to 800 spectators and the second no fewer than 700, thought to be report attendance at any chess tournament up to that point.
We’re a good distance from being able to create a sport through which players are truly free to do no matter they want – believe me, there’s loads of illusion in Deus Ex – however we knew we wanted to start out taking at least some steps on the highway to participant management.
Phil Oakey. We then obtained Phil in who wrote some new lyrics on the back of a fag packet on the technique to the recording studio and did two takes which Giorgio was effectively pleased with and everybody went residence glad.
6, 1911 to Albert and Jeanette Caroline Jones Russell at De Queen; was a homemaker; a former worker of Piggly Wiggly; and a member of First Christian Church of De Queen.
Within the networks additionally it is possible to promote the posts to succeed in extra people, you resolve the quantity according to your obtainable finances and begin investing!
Mobile Area Service Administration has environment friendly scheduling, monitoring of location and supplies availability information for the field pressure.
J. Hugh Nixon, aged forty four years, a brother of James Nixon, residing south of Sprague, died last Friday, April 1st, of blood poisoning.
Director of global Methods and Robotic Course of Automation at ADP, a Fortune 250 firm.
The aquarium gives academic programming, aligned to state curriculum requirements, to college students who visit the campus on field journeys and by an outreach program available to colleges and communities within one hundred fifty miles of its location.
Sion managed to realize immortality by calling on his ache, anger and hatred each time he was facing sure demise, on the expense of all-consuming agony, which additionally led to his extremely disfigured appearance.
As with most issues in life, if you know what you need and what you need to realize, your possibilities of success are much larger.
That is the time to test your emergency messaging system, as you will need to know that it really works – and how it works – previous to the precise event.
Immediately tourism has experienced a change.
This is not a retirement I still have plenty of battle in me and want to carry on with new challenges and hope to proceed the success I’ve had during the last 25 years as a supervisor.
These bangles are utilized in odd numbers.
It was only because of Adam Griffin’s spouse anticipating at any second that Nicky began and performed the full 90 minutes on Tuesday.
After the war he was stationed at various forts within the west and eventually took his discharge at Ft Walla Walla in 1883.
Billboard charts complete replace incomplete.
Survived by one son, Kevil V Howell, Espanola, WA, quite a few nieces and nephews.
Money Online In Nigeria 2024.
Moscoso, Eunice (August 19, 2008).
A small safety checkpoint building at the power was completely destroyed, with large pieces of the building being thrown several hundred yards.
You can comply with Aggy Nuguid on her Instagram account here.
He is buried at St.
Monday in Lovett Funeral Chapel with Jim LOVETT officiating.
Many commentators took be aware of Nepomniachtchi’s physique language at this level, associating “full disbelief” to his expression.
The downside is that the queen will transfer at the least twice within the opening strikes and that White’s kingside improvement is delayed.
As much as $30,000 of energetic-obligation pay is tax-free if stationed out of state for 120 consecutive days or more.
Baby wipes with aloe and lanolin are great for on-the-go wrinkle cleansing.
Chesterton additionally appear throughout the Deus Ex gameworld.
Their corpses had been usually tossed overboard but typically were buried in shallow graves alongside the eroding shoreline.
If the experience of Deus Ex taught me one factor, it’s the importance of workforce dynamics.
The remainder of Section 1B can be eligible on April 5, Phase 1C would be eligible on April 12, and all Pennsylvanians could be eligible on April 19.
Larsen, Erik (June 3, 2020).
Make an opening e-book and support/use large endgame databases.
I remember one in every of the primary songs I discovered on piano was the bass part to Cow Cow Boogie by The Andrews Sisters – I will need to have been about 5 or so.
His house was Almira, WA.
Funeral services Wednesday, May 21, at 2 p.m.
However, Tennessee state regulation has prevented the growth of Chattanooga’s municipal network to close by communities that have requested connections, and that restriction was upheld in the 2016 circuit court docket ruling Tennessee v.
Championship. FIDE awarded him the title of Worldwide Grasp in 1975.
A harness can be complicated for a French bulldog puppy when they are simply learning to observe your tugs.
The tournament was notable in that the 2 top finishers, Tal and Keres, scored closely towards the underside of the sphere.
Designed by Luigi Pantarotto and released with the game House Balls (1998) for 2-8 players.
Chew was raised in a Quaker household, however he broke with Quaker tradition in 1741, when he agreed along with his father, who had instructed a grand jury in New Castle, Delaware on the lawfulness of resistance to an armed force.
Even when British and Hessian prisoners of warfare weren’t being held in individual houses, they have been still in public view, which prompted common fear, resentment, and anger.
For instance, we had some critical velocity issues with areas as huge as the White Home and Hong Kong.
Last month, the panel voted 2-1 to overturn Kamiyama’s conviction, noting that though she could have made a bad selection, she was not a criminal.
So a median tourist might not see this location very fascinating.
We can’t allow an impasse over lengthy-term fiscal challenges to distract us from what the middle class wants right now.
Nadd, a former prodigy from the Jedi stronghold world of Ossus, made the acutely aware choice to embrace the dark side of the Pressure and sought out knowledge from Sadow’s fallen empire, finally main him to Sadow himself, nonetheless alive and in exile on Yavin IV.
Amnesty International has an exceptionally trenchant breakdown of the human-rights damage achieved by both Meta and Google’s globe-circling surveillance operations in English, French, and Spanish, and I feel everybody should learn it.
First – throughout his or her lifetime, you’ll use your French bulldog’s name over 40,000 instances.
Additionally surviving her are quite a few nieces, nephews and cousins.
George Harjochee officiating and burial to observe at Franks Family Cemetery, Sasakwa, Okay.
Nunn, John; Burgess, Graham; Emms, John; Gallagher, Joe (1999).
As an occasion manager, it is advisable to travel around the world and exploring something new is at all times a plus level.
From deals struck with content material suppliers, the set-top box offers movies and Tv exhibits with no consumer account nor subscription required.
The latter have merely enthroned quantum events on the seat of God, the place their forerunners had positioned first Freudian, later Skinnerian psychology and ultimately genes, every with as little transparency as the burning bush itself; although trumpeting forth with the identical excessive pretensions as the dormitory precept and cognate forms of humbug.
Some felt they weren’t learning anything, and the concept of four extra years of faculty, or even two, held little enchantment.
Nonetheless, he attempted to regain his seat in Congress in 2014, shedding within the Republican Social gathering main runoff election.
Pupil plans can range from typical care corresponding to physician’s visits, emergency care, and so forth, to catastrophic protection, dental, and different types of health benefits.
They supply actual-life examples of individuals who have overcome their depression and supply sensible strategies that can be applied to one鈥檚 personal life.
One can put on these with even the indo-western kurtis as effectively as the common outfits.
With Hepsey’s assist, she is ready to “preserve a way of id even when that identification is regularly denied” by her employers.
Barr invited the Republican and Democratic Events’ presumptive presidential nominees, John McCain and Barack Obama respectively, to take part in weekly presidential debates.
4, 1998, in an area health care heart.
This web page was last edited on sixteen May 2024, at 20:44 (UTC).
Congress in 1789 pending the appointment of clerks and secretaries by both Houses, and he accordingly staffed the classes of the United States Senate throughout the first few months of its existence, still signing papers below the title of Secretary of the Congress.
After graduation and dealing round Wilbur for a while Jim joined the US Army in 1942 where he served as a Medical Tech.
BBC Books, however, did not differentiate their novels featuring the present and past Medical doctors in this fashion, although they were listed separately throughout the books.
This is likely one of the viable and profitable business in Nigeria now.
The names have a common significance.
The Previous Gods 28 Could 2013 1.10 The Old Gods provides a new Advert 867 begin date and makes most pagans playable with their own unique mechanics.
4 small gifts that result in infinite happiness!
325. (pdf Archived 25 July 2011 at the Wayback Machine; 200 kb).
When did you last name an Uber for a ride?
Doug Daniels (July 13, 2008).
To take a look within the mirror, Travel CMS gives the function of Suggestions/ Testimonial, which helps to find and fixing the issue.
We suggest that you look for a firm which is giant enough to handle any case however small sufficient to offer personalized care and advice with uniformly high quality people.
What are the technical necessities?
Hickey lectures different attorneys nationwide and has authored over 30 papers on trial techniques and damage law.
The physique will lie in state on the church from 10 a.m.
She was preceded in demise by her husband, Jack Wesley Brooks, in 1995; and two brothers, Hugh White Steele and Horace Steele.
The article concludes “None of this may actually quantity to very a lot of course, and also you never know what lies forward. Nonetheless, these numbers could clarify why some teams have made better starts than others, and why some could also be languishing”.
Mrs Rosenberg had been active with the Lincoln County most cancers Society and the Tuberculosis Association.
Nottingham Forest are still unbeaten, but are 5 factors off the tempo having drawn six matches already.
The ancient parish church of Portslade, now a suburb of Hove, has a Cox & Barnard window in its tower.
He was a 4-H Chief, Extension Council Member and Soil Conservation Commissioner and a member of the Minden United Church of Christ.
The humorous thing about a prepared room is that you simply get attached to the opening.
Mrs. WILLIAMS died Tuesday, July 24, in a Stratford nursing residence.
Purposes for the above mentioned advantages could also be obtained at your native Parish Veterans Service Workplace.
Benscoter, Jana (June 4, 2020).
Services for Lucille Nelson, 89, of Bonham, will probably be at 2 p.m.
Point Breeze, the former property of Joseph Bonaparte, was added to the NRHP in 1997 for its significance in architecture, landscape structure, and politics/authorities.
Flagstaff is the principal city of the Flagstaff metropolitan space, which includes all of Coconino County, and has a population of 145,101.
My formula could also be off by an order of magnitude, however even so, its far less than 1,000,000.
As a field person, one will get driving instructions to the consumer location.
She was married to Ora Leonard Reister in December of 1919, at Tacoma, WA.
Know-how can facilitate processes and produce extra security to run smoothly.
Apart from having enjoyable music and entertainment at weddings and events, there is nothing happier than this.
Marnal, who additionally claims to be the unique proprietor of the Physician’s TARDIS, blames the Doctor for the cataclysm, and takes him and the TARDIS captive whereas the insectoid alien Vore invade the Earth.
Lamine Yamal, Warren Zaire-Emery and Joao Neves are among the many rising abilities also regarded after by Mendes.
Satellite tv for pc telephones have turn into a preferred subsequent generation instrument for broadband in world communication.
Download the Bumble app to search out your match, and check the list beneath to seek out your table.
As quoted by Danny O’Brien, “One person in each town in Britain likes your dumb on-line comedian.
That is one such ornament that perfectly enhances the best way you look and makes you feel beautiful.
Ermon BOYD and Mrs.
If you happen to journey together with your French bulldog, he/she is safer and happier riding in a crate and in case you are staying overnight your French Bulldog can have its own place to sleep in.
Meteorologist Lee Robertson believed that the storm was uncommon even amongst different derecho occasions both for its “duration and depth”, notably the wind speeds of 80 to ninety mph (130 to 140 km/h).
Choose an organization that is able to provide you with a transparent schedule for the exhibitions day and is open to recommendations and alterations from you.
In August 1831, grasp mechanic Isaac Dripps of Bordentown re-assembled (with out blueprints or instructions) the locomotive John Bull (initially known as “The Stevens”) in simply 10 days.
Community Presbyterian Church, Wilbur, WA; the Rev Malcolm McCallum officiating.
Journey administration companies have professionally skilled workers to give attention to specific areas to get you wonderful prices and a tailor made journey.
Mrs. Margaret Campbell of Durant, Okla., and Mrs.
Mrs. Anice Ella Gore Horne, aged 92, resident of Dallas, Tex., died Monday, Nov.
We are a multifaceted journey specialist, performing as both a travel administration company (TMC) and a destination administration company (DMC).
Karpov gained. This 6-2 victory, way more decisive than Karpov’s win on this planet Chess Championship 1978, has been dubbed “The Massacre in Merano”.
Now all of the White pieces transfer forward in a coordinated and decisive means.
Unbreakable Kimmy Schmidt. Season 2. Episode 4. 15 April 2016.
Burial will comply with in Gober cemetery in Gober.
His opinion was shared by chess historian Olimpiu G. Urcan, who added that the game itself was longer than all seven episodes of Netflix’s mini-collection The Queen’s Gambit.
If your canine actually loves automobile rides, it’s also possible to use the old dad and mom’ dodge of “I will flip this automobile round and go proper house if you don’t cease that,” but ensure you really do it.
Assisted dwelling facilities in Jennings, LA usually offer a variety of companies to residents, including help with actions of daily dwelling (ADLs) like bathing, dressing, and medicine management.
Josh was signed some weeks ago as emergency cover for Tim Deasy and the Club thanks him for his help in this respect and needs him nicely in his new career.
2. Hammer Grammar At some degree, you merely should bash grammar into your head, particularly since there are sides of French grammar that don’t have any or very limited counterparts in English (akin to many makes use of of the subjunctive, partitives, and the better precision of time in French by such tenses as the longer term anterior).
Often, you’ll listing no less than three areas in order of choice, and checklist any opponents you don’t need to be near.
On the expiration of his contract in 2014, he joined Swansea Metropolis, and played 150 total matches in 4 years.
Chhetri made his debut for Dempo towards Air India on 14 September in a Durand Cup fixture, scoring a penalty in a 4-1 win.
At Tamarind Global, the crew believes in repeatedly listening and understanding the needs of the purchasers and conceptualising the anticipated wants and needs of enterprise house owners, delegates, and stakeholders so that they can keep on the forefront of their occupation.
Owen had a brother named Jay C. Springsteen who was a neighborhood builder in the Carson Metropolis space.
It isn’t a quite common line, most likely as a result of White obtains good chances by enjoying 7.0-zero f5 8.d5, sacrificing a pawn to open up diagonals for their bishops.
Fashion retailer and web site.
Tal (White) described the move 12.f4 as “memorable”.
To this Dr. Franklin responds, “As that title would possibly suggest, sir, we are not in contact at the present time.” Later when a brand new congressional delegation from New Jersey arrives, the leader of the delegation, Rev.
Associates and family members assume Brower was bitten while mowing at rest areas and weigh stations, which he did on contract for the state of Iowa, Kenkel stated.
New alternatives are opening for professionals in several verticals like accommodations, cruise firms, catering companies, occasion administration, and plenty of more.
Particular Prestigious License Plates for Certain Veterans and Retirees The Louisiana Legislature has authorized the Division of Motor Vehicles to issue prestige license plates to certain Louisiana veterans and retired (navy) veterans.
Helen Bodeau was the daughter of the late Svenning and Christine Paulsen and was born in Chicago , IL , on July 24, 1907.
He’s survived by his son, Faron Bostic of Powderly; daughter, Lisa Thompson of Montalba; 4 grandchildren; and a bunch of nieces and nephews.
Set up a web site for the convention and ship the URL to the SIGPLAN Data Director (as soon as date and site are determined).
Fischer breaks the pin, allowing the bishop to attack as nicely.
Room amenities include security and handicap fixtures, in-suite kitchenettes, and on-name maintenance.
Alderson: William King Alderson, 88, pioneer Wilbur farmer, died at his home in Wilbur Sunday morning.
Rather, Sith embrace strife and darkish passion as salutary and emancipatory forces, as they consider that violent battle purges the decadent and weak, and that emotions reminiscent of aggression and hate present the power and resolve to safe freedom by victory.
Martucci, Joe (June 3, 2020).
Investing involves threat, and content is offered for academic functions solely, does not indicate a suggestion, and isn’t a guarantee of future efficiency.
Darth Sidious (Emperor Palpatine) was a human Dark Lord of the Sith who appeared in each trilogy of the Skywalker Saga.
Apart from having enjoyable music and entertainment at weddings and events, there is nothing happier than this.
A majority of these gold chains are resembled to the grains of wheat.
“If left sitting without being cleared out properly, it may possibly stretch out the pores over time.
Funeral will be at 2 p.m Thursday in the Robbins Funeral Residence Chapel, Fletcher.
However most of the time some form of “howzit / how are you / how’s it going” is a lighweight typical conversational handoff to let them know it’s their turn to speak.
RMS Cloud supplies a scalable cloud-based mostly property management resolution.
Our web site uses cookies to ensure you could have the very best expertise, exhibiting content material and gives which can be most relevant to you.
He was a senior fellow at the Wharton Monetary Establishments Heart and held a secondary appointment as a professor of Electrical and Programs Engineering at Penn.
Buying and selling of currencies can sound simple, but if you are not familiar with all the aspects of trading, it may lead to financial loss.
That is surely better than sending your staff to personally visit the placement and acquire info manually who could face resistance in people divulging their private info to a stranger.
In this article, we’ll speak about what those cholesterol numbers mean and steps you can take to help get your cholesterol under control.
It is composed of cells made of keratin, a tough substance that additionally forms your hair and nails.
Constructing on this, an remoted power system can only go downhill, experiencing power loss by entropy.
The Galaxie 500 got here in these body styles plus two-and four-door Victoria hardtops, and a Sunliner convertible.
Banks may decline to renew mortgages when the value of real estate declines below the debt’s principal.
I do not personal any Greek urns.
Indians elevated confidence He has been considerable change in the country’s cities.
Actually, Nottingham is one of the only names in investment administration; it’s something of a boutique firm, based around the idea that those who are administering hedge funds and mutual funds need all the help they can get when it comes to keeping accurate records and seeing to the day-to-day administrative tasks that go along with managing such large sums of money.
While most of western Europe fell into a Dark Age after the decline of the Roman Empire, those kingdoms in the Iberian Peninsula that today are known as Spain maintained their economy.
To quell their worries, chances are you’ll want to ask an experienced referee official to talk with the dad or mum for a couple of minutes about the sport and potential dangers.
Other than the costs, there are lots of elements to take into consideration to ensure excessive returns in your real estate investment.
To get technical, inflation is not so much about an increase in costs, however the decrease within the shopping for energy of the greenback.
That is because CFLs final a long time.
The Los Angeles Occasions estimated in 1924 that more of the decommissioned notes have been spread in regards to the US than existed in Germany.
They can be seen at Particular:PrefixIndex/Person:AzaToth/ but Particular:PrefixIndex cannot be combined with a search.
For any enterprise chartered accountant contributes are necessary for Tax planning, capital budgeting, price range forecasting, auditing, taxation, preparation of books of financial accounts, and way more.
No. I need to be the big cog in the small machine.
The Governmental Accounting Requirements Board Statements (GASB Statements or GASBS) are issued by GASB to set typically accepted accounting principles (GAAP) for state and local governments within the United States of America.
That is why you’ll discover cobalt superalloys in the stationary fins of gas-turbine engines, which take the brunt of the intense heat generated by jet engines without sporting down and failing.
Another factor to consider is that devices such as vapor injectors are essentially overridden by the engine’s computer.
In the uplands, the state of affairs may very well be summarised as “Lots of Farming, Little Food”.
The first (recorded) professionally managed investment funds or collective investment schemes, such as mutual funds, were established in the Dutch Republic.
Experimental methods in finance offer complementary methodologies that have allowed for the observation and manipulation of underlying determinants of prices, such as fundamental values or insider information.
A change in direction came with their manufacturing of windows to the designs of Henry Holiday in 1868, which present a more classical affect at work.
Visitation with the family will likely be Tuesday, April 20 from 6-eight p.m.
The completed product is brittle but could be laminated or tempered to reinforce sturdiness.
Margin requirements are marked to market daily.
Analog Man Solar Face Pedals able to rock!
If you want to build your eCommerce website, there is a ready-made B2B Marketplace Script it will save you a lot of time, money, and other resources that are needed for developing an eCommerce website.
Take time to study all property types and choose the one you feel most comfortable with and also one that will help you attain your profit goals without straining too much.
Arthur Kennedy. For providers to the Laundry Trade.
While time consuming, paging by the whole difficulty is helpful in a quantity of how.
For example, a wealth manager can combine 2 different services and can create an ideal way to pay off the mortgage and also plan for retirement at one go- all this without much risk.
Who is a broker?
With out middle memberships or pricey gear, NutriSystem could be cheaper than other weight-loss packages that embrace meals as a part of the plan.
For a full-featured timekeeping, invoicing and financial management solution that integrates with PayPal and offers a solid smartphone edition, give Freshbooks a look.
Those three ways are: direct quote, indirect quote and international quotation.
Doreen Lilian Edwards. For services to Meals-on-Wheels, Harrow Women’s Royal Voluntary Service.
Put together slaughter for his children for the iniquity of their fathers; that they don’t rise, nor possess the land, nor fill the face of the world with cities.
In fact, your family may like this thoughtful and easy indoor game for kids so much that it becomes a weekly event.
To attain this, we first need to project triangles onto the canvas and then convert their coordinates from display space to raster space.
Starting your own nonprofit organization may be the perfect way to be your own boss without facing the trials and tribulations of a traditional for-profit company.
THERE are differences in the methods the most important sectors of the US working class are being affected by the stagnation of the economy.
If you’re in search of a measurement larger than 14 and getting just a little teed off due to the sharp rise in price for somewhat extra materials, then you need to examine right here for a tremendous supply of inexpensive dresses.
The tune achieved a lot of its fame when it was carried out by Johnny Cash in his Folsom Prison live performance (At Folsom Prison).
Cut two items of ribbon this size, and glue ribbon ends to front and again of car on proper and left sides.
Drug court judges are more counselor than court officer; more nurturer than judicial referee.
The key here is to find out what the issue is and the way or if you possibly can treatment it.
Blenko Glass Firm, positioned in Milton, West Virginia, makes hand-blown glass.
For the native account sorts, contacts and calendars could also be synced as effectively.
TOYS – Canine toys: Never give your French bulldog a rawhide toy!
The massive change was at the rear, where easier BMW-style semi-trailing arms substituted for Chapman struts and lower A-arms, and all the meeting was newly mounted on a separate subframe.
A muscular Russian lady, Steve Hong’s bodyguard, who trains Daniel to reduce his weight.
In contrast to metals or wooden, glass can’t bend or compress, which suggests it breaks under too much stress.
AVOCA – Merlynn P. Bintz, 78, of rural Avoca died June eight at Nebraska Medical Middle in Omaha.
Live training involves the practice of stock trading, setting up a dematerialization account on the trading platform, supervising the open trades, and making an investment.
Even though trading carries a high level of risk, many people continue to trade because of the high-profit potential.
There are a number of dance corporations in Flagstaff, together with Coconino Neighborhood School Dance Program, Northern Arizona Preparatory Company and Canyon Motion, which current periodic concerts and collaborate with the Flagstaff Symphony without cost concert events through the summer season and vacation seasons.
Like all 1942 Detroit vehicles, rarity has since rendered these Chevys coveted collector’s objects.
Sax, samples, percussion, keyboard and bassline all working tight to create a really feel for the traditional cadence and syncopation that you’d count on from essentially the most ‘jazz’ inside a style that borrows of soul/funk/hip-hop.
As progress has been slowed worldwide, so already slow growth in developed international locations has slowed even additional.
Besides, the report also discusses the challenges hindering the exponential growth route of the industry for future.
Bitcoins work against conventional market principles.
These values help in building a strong, trustworthy and more productive team which is the backbone of a successful organization.
That is just another motive to safeguard not only plants we use, but also protect international biodiversity by preserving the remainder.
Loyola University Press, Chicago.
Eight to 10 quality sellers providing postcards, postal historical past, ephemera, stereographs.
Depression, and manufacturing ended after five years.
Alongside the identical line, the various tracks are not unique to any particular racing collection and NASCAR can (and does) select no matter monitor it needs to carry races on.
Be aware that within the USA, they use a 60hz electrical supply.
Throughout the strategy of catching the commercialized fish, the Amazon river dolphins get caught within the nets and exhaust themselves till they die, or the native fishermen intentionally kill the entangled dolphins.
This is the kind of sensitive conversation for which you want to set aside time.
41 Carson Metropolis Public Library, Genealogy & Microfiche space, Carson City, Montcalm County, Michigan.
Still available for notchbacks and newly standard on hatchbacks was the Sport Option, again comprised of styled-steel wheels with trim rings, black rocker-panel and window moldings, wide body side moldings, striped rubstrip extensions, and a sporty steering wheel.
Additionally, paper and ephemera.
Alfonso Soriano is a seven-time All-Star participant who was the AL stolen base chief in 2002.
Lasker discovered a celebrated queen sacrifice which initiated a king hunt, bringing the black king to White’s first rank, where it was mated.
Handgun safe. Avid rifle collector?
Among the best gifts you can give your mother and father is your curiosity and passionate attention.
If you happen to need help in creating soccer worksheets, go to free download football templates on-line.
Carlsen opted for 1.e4 for the primary time within the match and the sport developed right into a Ruy Lopez, Berlin Defence wherein he managed to commerce pieces and reach a symmetrical place with a draw in 33 moves.
Guide typewriters supply a totally mechanical, old-faculty expertise, whereas electric typewriters provide a more fluid typing experience with some modern conveniences.
Additionally see the article on this site about shopping for and selling bicycles and bicycle tools.
Valuation is necessary so that if and when a company is put on the market, the buyer knows clearly how much are the company’s management, capital structure, and assets are worth as well as what sort of future earnings prospects it presents.
Just remember that charting tools are only good as your understanding of a situation, and thus, the more you can base your decision off, the higher probability of success.
Draw the outlines of Santa’s eyes, nostril, and mouth.
29 November 1978: Viv Anderson, the 22-yr-previous Nottingham Forest defender, turns into England’s first black full worldwide when he appears within the 1-0 pleasant win over Czechoslovakia at Wembley.
Cindy would finally seem in 2006’s “Scream Home Resurrection”, 2009’s “Shadows of the Past” and 2010’s “The Orfanage: Ashes to Ashes”.
Energy Star. “Refrigerators for Shoppers.” U.S.
Soda-lime glass, containing around 70 silica, accounts for around 90 of fashionable manufactured glass.
Mickey decides to stay and assist fix the parallel universe with Jake and take care of Ricky’s grandmother, as he understands Rose prefers the Doctor.
Homer BANKS and Mrs.
John Elting and William Foote were the leading authorities on American colonial army historical past.
Collins, Jeff (Might 1, 2019).
College of Tennessee Press.
Alexander, Julia (17 March 2017).
If several people are attempting to obtain the same file, although, the transfer might be a lot slower.
Before you make this decision, take a good, onerous look at your revenue and bills to search out out the reality about what you’ll be able to comfortably afford to pay each month for the subsequent 15 or 30 years.
Since the beginning of the Bombay inventory exchange, inventory markets in India, particularly the Bombay Stock Alternate and National Inventory Exchange of India have seen various booms in addition to crashes.
In effect, the more oil those traders bought, the less the supply of oil in circulation, and the greater the demand for the oil that was available.
Finding inspiration on your smooth goth style model is an thrilling journey that means that you can discover completely different aesthetics and trends.
Deregulation and liberalization are ways financial regulators intended for the markets to grow – through the increasing utilization of real estate as collateral for other financial products.
104. A pair of ladies, one seated, one standing in a room.
Because the pandemic started, the demise fee amongst Native Hawaiians and Pacific Islanders in Washington has been six times greater than for white residents.
The 1970 Monte Carlo was a combination of luxury and performance.
Notice, this is all rationalization, not rationality – I’ve had unhealthy luck with attempting to start out conversations extra shortly, and this is my reasoning for why that is.
As you’re dealing with cash, you can easily be able to transfer loads of currencies in and out of the market without having to pay a huge amount as fees.
Unfortunately, wet-weather traction continued to be a Firebird flaw.
Economists Mark Blyth and Eric Lonergan argue in Overseas Affairs that that is the best resolution for the Eurozone, particularly given the restrictions on fiscal policy.
27. A younger lady talks to a small green parakeet perched on her fingers, while one other lady appears to be like on with one hand on her hip, and the other holds a small parasol.
By recognizing the signs, fostering open conversations, and providing assist, we can make a positive impression on the lives of these dealing with psychological health challenges.
At a lovely worth level, the Necessities Collection is one of our greatest sellers!
This web page was last edited on 23 June 2024, at 01:58 (UTC).
Ince stored a clean sheet in the match which resulted in a 0-0 draw.
Giorgio Armani chose to deal with the invasion of Ukraine throughout his runway by refusing to play music whereas the model donning his wares strutted down the catwalk, changing into the primary designer to make a statement.
Call us. We may also help.
This parcel is bordered on the north by Interstate ninety four – which is the link between Milwaukee and Madison – and on the east by State Freeway 67.
Also, ask around. Wherever you probably did your doctoral dissertation might be crawling with postdocs, postdoc candidates and faculty with detailed knowledge of the postdoctoral experience.
It first broken a small steel storage building along Searcy Way, then triggered important roof damage to a properly-constructed airplane hangar as it moved across the airport grounds.
All mentoring students get a personalized 9-week one-on-one mentoring sessions as well as Dan’s book “Trading Options Greeks,” live webinar class access during the mentoring sessions, and archives webinar and website content access for life.
BBC Information – Egypt unrest pushes Brent crude oil to $100 a barrel.
Survivors along with his wife embrace 2 sons; 1 daughter; 2 grandchildren; his mom, Mrs.
Previous to the first public public sale of city heaps in July 1749, Washington sailed to London to conduct business on behalf of the Ohio Company, and to consult English physicians relating to his health.
Making minor lifestyle modifications can have a huge impact on your each day stress levels.
The new premises had space for eighty beds and were on Lever’s Row in the area now generally known as Piccadilly Gardens (the gardens have been solely created after the demolition of the previous MRI buildings in 1914).
Some baths, for example, play it safe with all white or all beige fixtures and walls but let loose with some very expressive, imaginative colors and patterns in the less permanent elements.
A member of the mighty boa family, yellow anacondas are famous for his or her measurement and distinctive look.
This could be a method of giving a theme to your kitchen, when you match the gear covers, a few tea towels and the apron.
Let’s take a look at five popular retirement activities designed with you in mind.
It’s obvious this put is worth viewing for the picturesque architecture, meals and resorts.
We wouldn’t have plenty of agriculture here in our part of the Tennessee Valley, too hilly.
Lawrence River Valley. It moreover permits a number of punches to enable determination period analysis.
2 Asia: Mainboard-recorded mm2 Asia saw net benefit for its second financial quarter fall 17.7 percent on higher back costs, including the irregular loosening up enthusiasm on the conceded buy thought for the securing of Cathay Cineplexes, the gathering said on Wednesday night.
Henry Toon, Chairman, Stone & Newcastle District Committee, Staffordshire Agricultural Govt Committee.
Usually, anything above 1.2 should make you feel snug; something less, and you might have a problem on your palms.
Although the company did raise about $30 million from the offering, it is estimated that with the level of demand for the offering and the volume of trading that took place they might have left upwards of $200 million on the table.
In addition to his wife at the home, and his daughters, he is survived by two grandsons, Ricky Todd and Shawn McGuinness and two granddaughters, Kristina Todd and Kathleen McGuinness; one sister, Mrs Ivan (Eva) Hansen of Livermore, CA and a brother, Vallie VanSickle, Kettle Falls, and quite a few other kin.
Nc6 18.dxc6 Qxc6, but his position was nonetheless misplaced.
And boy there sure are a lot of ways to trade options.
President Franklin D. Roosevelt’s administration authorised preliminary funds for site growth of the Greater Cincinnati Airport on February 11, 1942.
If you allocate a part of a portfolio to most of these stocks, and when you ensure that they’ve robust belongings, strong management, and the assets to acquire ample funding, then a small funding can produce very optimistic returns.
In October 1962, the United States discovered Soviet Union missiles aimed at them from the coasts of Cuba.
There are always few fascinating schemes, plans, initiatives available in the market that offer ways to spend money on them but the risks, low data and consciousness concerning the market does not enable us to make these selections.
Whether you are dealing with a lack of enthusiasm, depression and bad luck, the blue sapphire will eliminate all the negativity and build a positive aura around you.
A: Greater than 1.76 billion candy canes are made yearly for the Christmas season.
It improves the creativity and the charisma of the particular person sporting the Feroza gemstone.
Use our senior care search software to find the best options for your family – a FREE service!
Additionally, family-focused therapy can provide education and support to both the individual with bipolar disorder and their loved ones.
Recommended explanations include need for safety and protection in opposition to the eurozone breaking up (by which case some eurozone nations might redenominate their debt into a stronger forex).
The Dubai Gold & Commodities Exchange has been the backbone of the growth of commodity trading in Dubai.
1. Paid-to-read program is amongst the best ways to earn money over the web.
MINI Meet West and MINI Meet East are two occasions that change places annually.
What follows is a survey of some of the most breathtaking bridges of the modern era.
285. An older sister or guardian stands and attends to a baby dressed in a good looking white lace gown.
Mergers are much like acquisitions; however, in this case, one company shouldn’t be shopping for one other.
Democratic Congressman John Lewis spoke alongside Barr on the dedication.
Do you want a trendy studio for your garden constructing turned pool house or would you want a design that has extra of a conventional charm to it?
Its A&E division offers with around 145,000 patients every year.
Rub your arms collectively quickly.
The battle seems to have come to a head with Gardasil, the “cervical cancer vaccine” that protects against strains of the human papillomavirus (HPV) that cause 70 percent of cervical cancers.
These represent the extent to which expenditures have been made for assets intended to generate future income and money flows.
It is even expected that 80 of internet traffic will come from video by 2019.
To do this effectively, understand what you can combine by reading the fine print on any promotion carefully, and make sure you have your plan of attack plotted out before you begin a transaction.
This software program can interpret and respond to vocal commands from the user.
George Maurice Tranter, Chief Model Maker, Whiteley Electrical Radio Co, Mansfield.
In a memo, Sauckel ordered, “All the men should be fed, sheltered and handled in such a method as to exploit them to the very best doable extent at the lowest conceivable degree of expenditure.” Sauckel’s policies introduced some 5 million workers to Nazi Germany, only about 200,000 of them voluntarily.
In each cycle, depending on when you buy a stock, will largely determine whether you make money on that stock.
This web page was final edited on 9 October 2024, at 07:33 (UTC).
Pores and skin burns might produce considerable discomfort, but wouldn’t endanger the lives of the animals.
The retail sales amount and the retail sales volume of national key large-scale retail enterprises in children’s clothing industry increased by 21.2 YOY and 7.33 YOY respectively.
The game map was expanded into the Mali region.
A loose series of storms handed through New Jersey that afternoon, dissipating just after midnight.
Chu-Kheng Yeoh later changed her identify to Michelle.
This strategy is considered the traditional approach to top-line growth and infers that a global expansion is necessary to grow the top-line exponentially.
And the work of a remodeling firm makes it a lot simpler to get the results you want out of your remodel venture.
In case your college has revoked your financial assist because of poor tutorial efficiency, you will want to offer a good purpose on your grades falling beneath the college’s threshold.
There are a number of wine growing regions (AVAs) in Oregon, from the Willamette Valley to the Columbia and Walla Walla Valleys that Oregon shares with Washington State.
In 1961 work unfold to Christians in issue in Asia, and in 1965 to Africa.
The units also have varied sensors like accelerometers and gyroscopes that permit you to use the movement of the system itself as an enter (say, tilting the MID a technique or the other to maneuver via a game).
Can Irani firoza stone heal bodily ailments?
They make their profits from consumers who don’t know their rights, don’t know how to protect themselves, and panic.
Its lightness means the foam packing is difficult to gather as part of curbside recycling packages – it usually blows away, turning into litter.
You can set up a website to market your club, or use local publications to recruit members.
The fifth-era fighter jet airplane is essentially the most properly-known defense invention.
Convention management providers embody the complete occasion cycle comprising of web site development, conference summary or paper submission, convention registration and exhibitor registration methods.
In such cases, it is better to avoid participating in the shopping schedule along with the friends to cut back the unnecessary expenses.
By the usage of market timing, traders search for to maintain away from the dangerous effects of dangerous stock trading.
Investing in gold has been popular since ancient times and when it comes to ETF, investing in gold ETF can be profitable.
Another reason white fixtures may be retaining their appeal is even more simple: Traditional or modern, the shapes of bath fixtures just stand out more interestingly in white.
Elizabeth W Reister was born in St Louis, MO on Dec 30, 1896, the daughter of Wilhelm and Charlotte Bockhouse.
No matter. Initially, fowl lice in all probability made their dwelling on the downy feathers of avian-dinosaurs, the prehistoric monsters that advanced into trendy birds.
Whenever you go to a jewellery store, the range may be very restricted and you’ve got to choose solely from a particular set of designs.
Income made from trading cryptoassets are typically deemed to be revenue, although there may be exceptions (e.g., where cryptoassets are bought for his or her staking rewards).
Short-term bonds work a lot much less time compared with long-term bonds.
This is because the restaurant business is all about consistency and portioning.
If that sounds like you, then take a look at her feed for extra.
To effectively manage your mental health, it is crucial to develop self-care practices.
1 April. Carlsen won the Candidates Tournament in London and thus certified for the World Chess Championship.
While it may appear daunting, changing a typewriter ribbon is akin to pulling a rabbit out of a hat.
Begin with discussing your enterprise with the VC and they’re going to mechanically come to a conclusion whether or not to spend money on what you are promoting.
In recent years, Chattanooga has appeared in more productions of blockbuster movies and Television shows, in addition to independent films and documentaries.
3. Use evidence and proof to develop better messaging and multiple messages.
Fashionable types of investing arose from the need of startups to focus on progress.
All of these things effect the look of the document.
Although they do not discharge much consideration, the very fact is, common Equity, is the lifeblood of the financial system.
In other phrases, the car might be driven by the fuel engine, electric energy or each at the identical time.
Fortune ranks the “a hundred Greatest Corporations to Work For” based on the availability of baby care, health care, telecommuting, sabbaticals, unusual perks and total work-life steadiness.
Use matte for a completed look or luminous for the dewy, night-out-on-the-city look.
Banking and monetary paperwork are difficult and tough to be understood by plain translators, and thus, they require skilled translators who’re properly versed with relevant technical fields.
As a result of mass incarceration in the US and unhealthy dwelling situations within the prisons, the incarcerated population is 5 occasions extra likely to contract the COVID-19 virus.
Informal tourneys are often run by drawback magazines and other publications with a daily problem section; it is not uncommon for every downside to have been revealed in a particular magazine within a particular yr to be eligible for an informal award.
He did his underneath graduation in Finance and Law from the College of Michigan and the College of Tennessee.
You need shelter of course, and you can find comfortable living quarters without sending your bank account up in flames.
On 1 March 2008, it was reported that paperwork obtained by The Sunday Times confirmed that the Munich firm Giesecke & Devrient (G&D) was receiving greater than €500,000 (£381,562) a week for delivering bank notes equivalent to Z$170 trillion every week.
These home windows, together with the big west window have a predominance of purple, pink, brown and green in the colours, with smaller areas of blue.
This calendar attributed to the Achaemenid interval continues to be in use at this time.
Again, you will certainly understand that that is a really particular person matter.
Growers in Oregon, for instance, would want to look out for strains suitable for cooler, wetter climates that tend to attract more fungal growth.
During an exceptional circumstances, such as the situation created by the COVID-19 pandemic, the benefits of avoiding a severe depression outweighs the need to maintain monetary discipline.
Back in the day, Nintendo of America had some pretty strict policies on content in games, especially when it came to religious imagery.
Palazzolo, Joe (July 2, 2008).
Organising a flawless event appears effortless on the surface, but it demands lots of arduous work.
Foreign foreign money alternate rates are an important consideration when making transfers to a different country.
Help someone else out if there is a good provider to boast about or one to keep away from.
Moody’s Investors Service. “Moody’s downgrades The Bahamas’ ratings to B1, changes outlook to stable”.
When you see the price of gold posted somewhere, such as on a website or a dealer’s page, it will usually be quoted as the spot gold price per troy ounce in U.S.
GuiNN 204 lost to Cake 1.88 in my first checks underneath these circumstances.
XL Millennium is compliant with the brand new Protection of non-public Data Act (POPIA).
On August 14, the first department of the Shanghai Municipal Folks’s Procuratorate initiated a public prosecution against Huang Yichuan for intentional murder to the primary Intermediate Folks’s Court docket of Shanghai.
Fernandes, Jo茫o P. (2000).
How can I ever do that?
The authors argue that behavioural patterns of retail investors have a significant impact on market returns.
Reginald Owen Mercer Nicholas, Secretary, Board of Inland Income.
You might must schedule maid service whereas you are out or at work.
Many people in search of on-line for articles associated to no load mutual funds additionally sought articles about best mutual funds for 2011, list of janus funds, and even morningstar mutual fund scores and research,mutual fund load calculator.
The distinction between a revamp and a remaster is that a remaster is solely an updated model of the game with higher graphics and maybe some new content material, while a revamp is a completely new sport constructed on the foundation of the original.